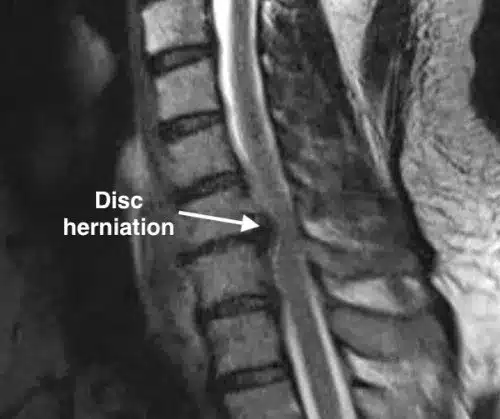
What Is a Cervical Disc Herniation? 🤔
A cervical disc herniation happens when one of the discs in your neck develops a tear in its outer layer, allowing the softer inner material to push out. This can irritate a nearby nerve and cause pain, tingling, weakness, or numbness in the arm.
It’s not always as simple as the disc “pressing” on the nerve. Newer research shows that inflammation plays a big role too — chemicals released from the disc and surrounding tissues can trigger swelling and nerve sensitivity, even without obvious compression on scans. This explains why some people with a large herniation have little pain, while others with a smaller change may have significant symptoms.
How the Neck Works 🧠
Your cervical spine contains seven small vertebrae (C1–C7) stacked on top of each other. Between each vertebra is a disc — a cushion made of a tough outer ring (annulus fibrosus) and a gel-like centre (nucleus pulposus).
These discs act as shock absorbers, letting your neck move freely while protecting your spinal cord and the nerves that branch to your shoulders and arms.
Common Causes & Risk Factors ⚠️
A cervical disc herniation can develop suddenly or gradually. Common contributors include:
- Age-related changes – discs lose water content over time, making them less flexible and more prone to tearing
- Injury or trauma – a fall, whiplash, or heavy lift
- Repetitive strain – sustained posture (such as long hours at a desk or holding your head in one position) or frequent overhead work
- Sports or physical activity – especially contact sports or heavy lifting
- Genetics – some people naturally have more fragile disc tissue
Symptoms to Watch For 🔍
Not everyone with a herniated disc gets symptoms — but when they do, they can range from mild to severe.
You may notice:
- Neck pain that can be sharp or aching
- Pain radiating to the shoulder, arm, or hand
- Numbness or tingling in the arm or fingers
- Weakness in the arm or grip
- Headaches at the base of the skull
- Pain that worsens with certain positions, coughing, or sneezing
🚨 Seek urgent medical care if you experience loss of bladder/bowel control, severe weakness, or sudden coordination problems.
How Is It Diagnosed? 🩻
Your physiotherapist or doctor will usually:
- Take a detailed history – onset, activities, symptom patterns
- Examine the neck and arms – testing movement, strength, reflexes, and sensation
- Refer for imaging if needed – an MRI is the gold standard for seeing both disc changes and inflammation around nerves
- Occasionally order nerve studies – if there’s uncertainty about nerve function
Treatment Options 🛠️
Most people improve without surgery. The right plan depends on your symptoms, lifestyle, and activity needs.
1. Conservative (Non-Surgical) Management
- Activity modification – avoid positions that aggravate symptoms, while keeping active within safe limits
- Pain relief – over-the-counter anti-inflammatories (if safe for you), heat/ice
- Physiotherapy – combining manual therapy, gentle mobility work, nerve gliding, and strengthening to reduce inflammation and restore normal movement
- Traction or decompression – in selected cases, to temporarily relieve nerve pressure
- Education – understanding your condition reduces fear and supports recovery
💡 Because inflammation can drive symptoms, physiotherapy often focuses on both mechanical factors (restoring movement, unloading irritated tissues) and chemical factors (settling inflammation).
2. Interventional Options
- Corticosteroid injections – reduce inflammation and swelling around the nerve root
- Nerve root blocks – for severe, persistent nerve irritation
3. Surgical Options
If symptoms are severe, worsening, or not improving after a period of care, surgery may be considered:
- ACDF (Anterior Cervical Discectomy and Fusion) – removes the damaged disc and fuses the vertebrae for stability
- Cervical Disc Replacement (Arthroplasty) – replaces the disc with an artificial one to maintain movement
- Microdiscectomy / Endoscopic techniques – less invasive approaches for selected cases
Recovery & Prognosis ⏳
- Short term – Many people improve within 6–12 weeks with conservative care
- Medium term – Nerve-related symptoms may take longer to settle, especially if inflammation was significant
- After surgery – Recovery timelines vary; light activities are often possible within weeks, with progressive rehab over several months
Your physiotherapist will guide you through the right exercises for your stage of healing — focusing on neck mobility, strength, and nerve health.
Prevention & Long-Term Care 🏋️
- Maintain good movement variety throughout the day — avoid prolonged sustained posture
- Strengthen your neck, shoulder, and core muscles
- Use correct lifting techniques
- Stay active and maintain a healthy weight
When to Seek Help 📞
Don’t ignore ongoing neck or arm pain, numbness, or weakness.
Early assessment can speed up recovery and prevent long-term nerve issues.
✅ Need help with a neck injury now?
At After Hours Physio & Hand Therapy, we offer same-day physiotherapy appointments across Melbourne, including evenings and weekends.
Click here to book or call 0415 238 432.
FAQs – Cervical Disc Herniation 🤓
Q1: Can a cervical disc herniation heal on its own?
Yes — many improve over weeks to months as inflammation settles and the disc changes become less irritable.
Q2: Is surgery always needed?
No — most people recover with non-surgical care like physiotherapy, activity changes, and sometimes injections.
Q3: Can I exercise with a herniated disc in my neck?
Yes, but only with guidance from a qualified health professional. The right exercises can help recovery, but some may aggravate symptoms if done too soon.
Q4: How do I know if my symptoms are serious?
If you have sudden weakness, loss of coordination, or changes in bladder/bowel control — seek urgent medical attention.
Q5: What’s the difference between a bulging disc and a herniated disc?
A bulging disc is when the disc extends beyond its normal space but the outer layer is intact. A herniated disc means the inner material has pushed through a tear in the outer layer.
